MIPSpro
Healthmonix users avoided $800 million in penalties and found over $300 million in incentives and shared savings in 1 year!
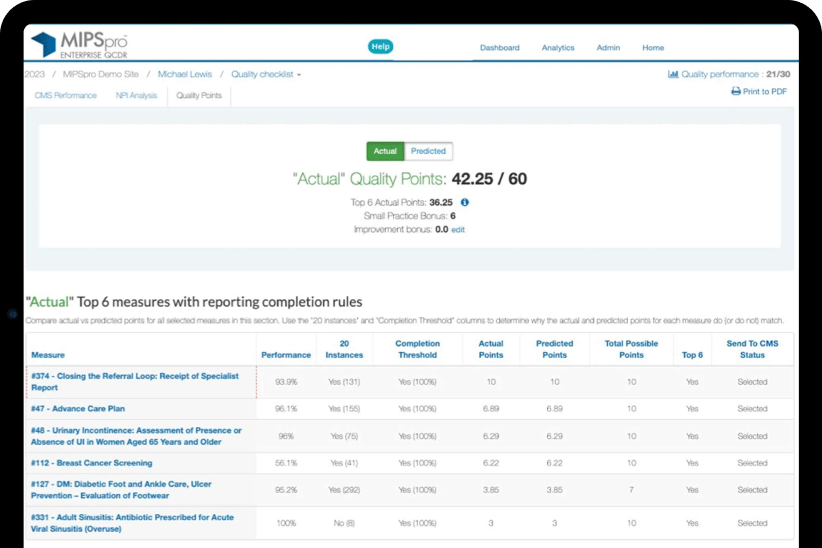
Succeed with MIPS reporting today and tomorrow
Selecting the right MIPS registry partner matters.
Healthmonix registries saved customers over $800 million in penalties in 2024 reporting. In addition, we secured them over $300 million in incentives and shared savings. Our registries and associated services are designed to help providers enhance their financial outcomes within the MIPS framework.
Our team of seasoned value-based care experts has been engaged with the MIPS program from its beginning. Their expertise has been pivotal in the creation of MIPSpro, our state-of-the-art product designed to elevate your MIPS score and maximize Medicare reimbursements.
MIPSpro is more than just an application; it’s a comprehensive toolkit that includes seamless data integration and strategic score optimization features. It’s engineered to optimize your MIPS reporting and submission process. Discover how our solutions can be leveraged to help you meet and exceed your MIPS goals.
Financial outcomes MIPSpro customers have achieved include:
$250K
A mid-sized orthopedic group improved their MIPS score from 68 to 100. With annual revenue exceeding $3 million per CMS reporting, they turned a potential $21,000 penalty into a $250,000 incentive within a single year.
$850K
A pain clinic transitioned from facing penalties before using MIPSpro to securing an $850,000 incentive.
$1.1M
An oncology group with 5 providers earned a full 8.25% incentive for their 2022 reporting, resulting in an anticipated incentive of $1.1 million.
$233K
A dermatology practice with 8 providers is on track to receive a $233,000 incentive for their 2022 reporting.
179%
A large hospitalist and emergency department organization with 40-plus TINs saw their scores surge by 179% in a 2-year span.
$800 million
MIPS shouldn’t be a gamble. In 2024, we protected our clients from over $800 million in potential penalties. We provide a frontline defense for your bottom line, ensuring every submission is valid and secure.
96%
Reporting is complicated; your partnership shouldn’t be. We’re proud of our 96% CSAT rating, a testament to our commitment to providing expert guidance and proactive support at every stage.
1.7 hours
Regulatory deadlines wait for no one. Our dedicated support team resolves technical and program inquiries in an average of 1.7 hours, giving you the answers you need to stay on track.
Advantages MIPSpro has over other MIPS registries
Healthmonix has supported clinicians’ CMS quality reporting, performance improvement, and population health management since 2009. We offer a user-friendly reporting solution so you can focus on patient health and improvement.
Enjoy a return on investment
The proprietary MIPSpro measure and scoring engines deliver a higher score than other registries and your EHR. MIPSpro can analyze all your data, find measure data other registries can’t, and provide flexible reporting options. This can increase your quality measure scores, leading to a higher return on your reporting fees.

Capitalize on advanced analytics engine
Our advanced analytics engine allows us to find the best reporting options for your organization. You’ll also receive actual score previews instead of predicted totals.
Whether it’s helping you determine your top measures or decide whether to report as individual NPIs or as a group, we’re focused on maximizing your MIPS score.

Identify gaps in care quickly
MIPSpro quickly reports gaps in care that can be closed by providers. By targeting identified patients, providers both raise their MIPS score and improve care to patients.

Reduce burden
Our relationships with leading EHRs allows us to establish integrations quickly. Once data is flowing into MIPSpro, gaps in data can be identified and closed.
Benefits to choosing MIPSpro

See real-time updates
Review live performance updates to make timely decisions to close gaps in care. Our measure, patient, and provider dashboards, along with advanced analytics, support targeted improvement.

Report all MIPS categories
Track the Quality, Promoting Interoperability, Improvement Activities, and Cost performance categories, something only MIPSpro can do.

Submit data to
CMS easily
With a few clicks, providers and practices can submit final data to CMS. Forget the burden of creating files to upload to CMS portals.

Contact U.S.-based support
Get quick, easy-to-understand answers from our highly rated Customer Support team.

Enjoy year-round reporting
Start reporting year-round with quality measures that are available during each performance year. Our proprietary algorithm selects measures to target and report for the optimal score.

Use integrated data
Report from 1 or multiple EMRs through flexible data-integration options. Use our patient matching technology to combine data successfully. Avoid manual data entry.